
Artificial intelligence training: Residents receive real life experience with realistic fake patients at the new Cape Fear Valley Health learning facility
By Eddie Velazquez, posted Mar 2, 2023 on BizFayetteville.com
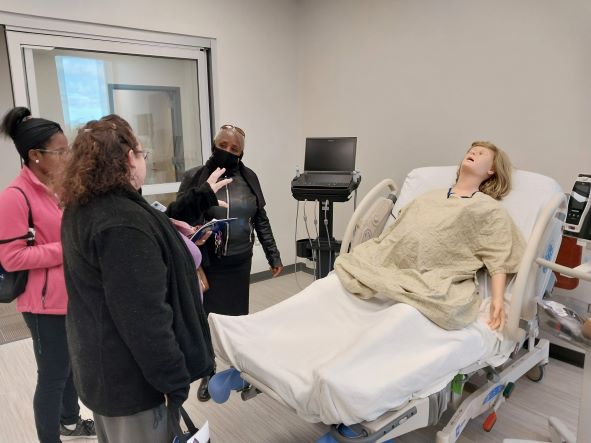
AI patients found in the CFVH Center for Medical Education and Neuroscience
Institute include a pregnant patient (pictured above), a grown man, small child,
toddler, and infant. All can simulate real life medical conditions, breathe, and
respond to their caretakers.
A partnership between Cape Fear Valley Health Center and a major pioneer in medical simulation technology could train and help retain the next generation of professionals in the medical field.
Medical simulation technology developed by Miami-based Gaumard Scientific is a main focus of the new Cape Fear Valley Health Center for Medical Education and Neuroscience Institute, which officially opened in January. The long term project was around 10 years in the making and was built in the last year and a half on the corner of Owen Drive and Melrose Road in Fayetteville.
Administrators have said in the past the hospital has offered 15 educational programs for more than 300 residency seats. Now with a new simulation lab on the third floor, residents can get hands-on training in surgery, emergency/ trauma treatment, labor and delivery and more thanks to new developments in artificial intelligence.
“Simulation really breaks down into a few different areas and it's really designed to allow physicians and nurses to train before they get involved with real patients,” said James Archetto, Gaumard’s vice president. “We have these very realistic, lifelike simulators. They're very human in terms of how they perform physiologically and the immersion that allows for students.”
The AI patient simulations at Cape Fear Valley Health can weigh up to 130 lbs and allows the use of real medical equipment, which familiarizes learners with the tools of the trade.
“That means the same electrocardiogram (EKG), the same blood pressure monitor, the same pulse oximetry monitor can all be attached to the simulator. The simulated patient actually has software and hardware that allows it to generate these signals that mimic the actual signals that the body makes.”
“They bleed real, they cry real tears, they sweat, and they speak,” Archetto said.
Archetto used the example of a patient that comes into the emergency room with chest pain.
“That simulated patient can be put on a real EKG and be defibrillated with real energy,” he said. “Let's say that [the] patient then had a heart attack. That same simulator could be moved into the critical care area and the students then could be checking arterial blood gas samples on that patient. They can hook the simulated patient up to real monitors in the critical care unit.”
According to Archetto and CFVH, the state-of-the art simulation technology can help address significant issues that plague the health care sector in the United States.
“There is no doubt that we hear about the health care shortage daily. There's a shortage of nurses, physicians, and first responders in the U.S.,” he said, noting that there are several bottlenecks that contributed to the staffing shortage issue. “One is that there aren’t enough people entering the workforce. Number two, is that there aren’t enough faculty to train those students.”
By 2033, the University of North Carolina (UNC) estimates that the state will face an estimated shortage of nearly 12,500 registered nurses. According to a study by UNC, the largest shortfalls for registered nurses are projected to occur in hospitals where demand could exceed supply by nearly 10,000 positions by 2033.
The second largest projected shortage of registered nurses is forecast to be in nursing homes and extended care and assisted living facilities. The shortage at these facilities by 2033 could be nearly 2,000, which is 31 percent of the workforce.
To decongest these bottlenecks, Archetto said, simulation can help get hands-on experience for students quickly.
“The technology allows you to reimagine that student-to-faculty ratio,” he noted. “You can have these autodidactic students who can go into a simulation center, learn at their own pace, and gain this very immersive educational experience without having to have an educator dictate to them exactly what's supposed to take place. It can be self-directed learning and simulation certainly helps in that regard.”
Archetto described the differences between didactic education and practical education. Didactic education, he noted, refers to students sitting in a classroom, listening to a lecture and later preparing for an exam.
“Certainly that is a way to learn conceptually,” he said. “Over the years, what we've learned, clinically, is that students retain far more information when they're actually able to practice these skills over and over.”
One of the lessons in education, brought by the distancing and spatial restrictions ushered in by the COVID-19 epidemic, is the notion that lectures aren’t exclusively confined to a lecture hall. Similarly, Archetto said, the pandemic also brought into focus a reimagining of hands-on training.
“With the pandemic, students were no longer allowed to go into hospitals for practical and clinical education of practicing on real patients,” he said. “Our technology allowed students to go into a simulation center that was very clean, not worrying about any COVID-19 contamination, and practice very sophisticated skills on a simulator.”
Simulation can also help open the doors for students of all backgrounds.
“You can set up a simulation center really anywhere and access to health care is a substantial problem,” Archetto said. “Access to health care education compounds that problem. Simulation centers can be remote. People don't have to go to large teaching institutions for education anymore.”
As an example, Archetto said simulators can be stored in a car and transported anywhere.
“There are educators that take their programs to very rural locations and this allows medical education to take place anywhere, which provides that access that in the past wouldn't have been available with typical clinical education.”
But the technology hasn’t always been there. In fact, Archetto said, it wasn’t until about 15 years ago that medical simulation technology experienced big breakthroughs.
“One of those is the ability for simulated patients to become wireless and tetherless, which is exclusive to Gaumard. Not all medical challenges take place in a hospital,” Archetto added. “Learners need to experience emergencies where they take place, whether that's on a battlefield, or a car accident.”
Gaumard’s simulated patients operate via a battery and are controlled via bluetooth, Archetto said, instead of being plugged into a wall.
“We're at this level of sophistication, where you're asking the simulator questions. They are answering you, they will squeeze your hand and are hooked up to real equipment,” he said. “Technology is used as a tool to allow us to ensure that the next generation of healthcare providers have the competency that they need to care for patients.”
Copyright © 2026
Enhanced Media Management Inc. dba
Greater Fayetteville Business Journal
This story may be displayed, reformatted and printed for your personal, noncommercial use only and in
accordance with our Terms of Service located at https://bizfayetteville.com/useragreement.